 Indeed, it is quite common for classic PNH to evolve from acquired AA, but well documented cases of PNH arising from MDS are virtually nonexistent. 34 It is possible that many of these patients have moderate AA rather than hypoplastic MDS (hMDS). MDS patients reported to possess PNH cells tend to be classified as refractory anemia and often have the following characteristics: a hypocellular marrow, human leukocyte antigen (HLA)-DR15 positivity, normal cytogenetics, moderate to severe thrombocytopenia, and a high likelihood of response to immunosuppressive therapy. 
GPI-AP-deficient cells (usually < 1% of granulocytes) have also been reported in patients with myelodysplastic syndrome (MDS), 14, 34 but sequencing of the PIG-A gene to establish clonality has not been performed in many of these studies. Because granulocytes and monocytes have a short half-life and are not affected by blood transfusions, the percentage of PNH cells in these lineages best reflects the size of the PNH clone. Solely screening red cells for PNH can lead to falsely negative tests, especially in the setting of a recent hemolytic episode or a recent blood transfusion. 24, 25 Ideally, at least 2 different monoclonal antibodies, directed against 2 different GPI-anchored proteins, on at least 2 different cell lineages should be used to diagnose a patient with PNH. It is noteworthy that rare congenital deficiencies of CD59 and CD55 may lead to a false-positive test for PNH if only one monoclonal antibody is used. 22, 23 CD59 is most commonly assessed because it is expressed on all hematopoietic lineages CD55 is also commonly evaluated. Most laboratories now use flow cytometric evaluation of specific GPI-anchored proteins because of its high sensitivity and specificity. 21 These erythrocyte-based assays do not reliably quantitate the percentage of PNH cells and can be falsely negative in patients who have received red cell transfusions thus, I no longer use these assays. The original assays to detect PNH erythrocytes included the Ham test, 19 the sucrose hemolysis test, 20 and the complement lysis assay. Patients with a Coombs-negative hemolytic anemia, AA, refractory anemia, and unexplained thrombosis in conjunction with cytopenias or hemolysis should be screened for PNH. Thrombosis is the leading cause of death, but others may die of complications of bone marrow failure, renal failure, myelodysplastic syndrome, and leukemia. 9-12 The median survival is 10 to 15 years, but with a wide range. The natural history of PNH is highly variable, ranging from indolent to life-threatening. Free plasma hemoglobin scavenges nitric oxide and depletion of nitric oxide at the tissue level contributes to numerous PNH manifestations, including esophageal spasm, male erectile dysfunction, renal insufficiency, and thrombosis. 8 Intravascular hemolysis releases free hemoglobin into the plasma. 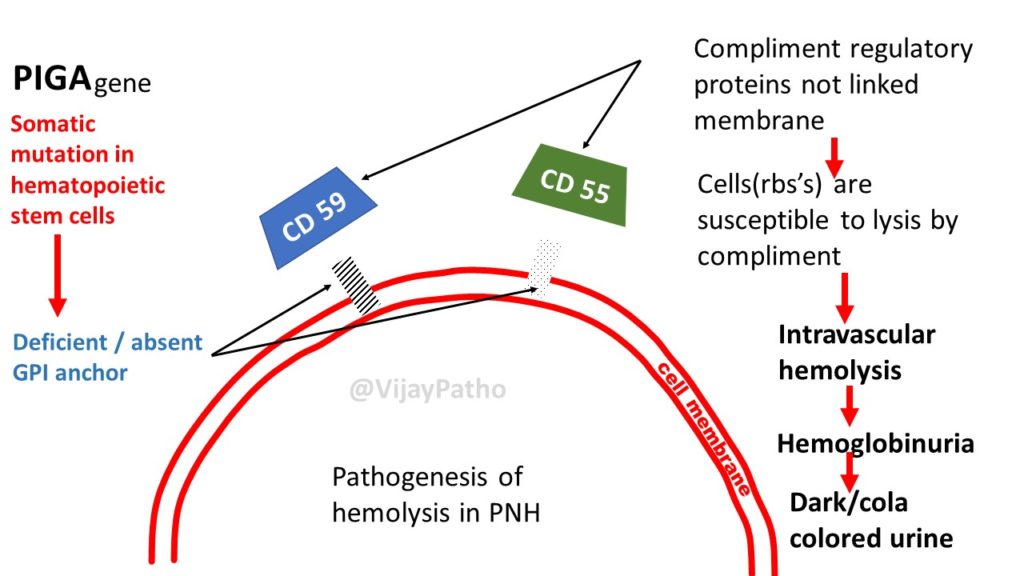
The loss of complement regulatory proteins renders PNH erythrocytes susceptible to both intravascular and extravascular hemolysis, but it is the intravascular hemolysis that contributes to much of the morbidity and mortality from the disease. 6, 7 CD55 inhibits C3 convertases and CD59 blocks formation of the membrane attack complex (MAC) by inhibiting incorporation of C9 into the MAC. Two of these proteins, CD55 and CD59, are complement regulatory proteins the absence of these proteins is fundamental to the pathophysiology of the disease. 
Consequently, the PNH stem cell and all of its progeny have a reduction or absence of glycosyl phosphatidylinositol (GPI)–anchored proteins. The PIG-A gene product is required for the biosynthesis of glycophosphatidylinositol anchors, a glycolipid moiety that attaches dozens of proteins to the plasma membrane of cells. 4, 5 Expansion and differentiation of the PIG-A mutant stem cell lead to clinical manifestations of the disease. 3 The disease originates from a multipotent hematopoietic stem cell that acquires a mutation of the PIG-A gene. 1, 2 PNH can arise de novo or in the setting of aplastic anemia (AA). Paroxysmal nocturnal hemoglobinuria (PNH) is a clonal hematopoietic stem cell disease that can present with bone marrow failure, hemolytic anemia, smooth muscle dystonias, and thrombosis. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
